Yes: if the patient can talk, their airway is patent and you can move on to the assessment of breathing. Airway Clinical assessment Can the patient talk? If the patient is unconscious or unresponsive, start the basic life support (BLS) algorithm as per resuscitation guidelines. Make sure the patient’s notes, observation chart and prescription chart are easily accessible.Īsk for another clinical member of staff to assist you if possible. Introduce yourself to the patient including your name and role.Īsk how the patient is feeling as this may provide some useful information about their current symptoms. Introduce yourself to whoever has requested a review of the patient and listen carefully to their handover. You may be asked to review a patient with pneumothorax due to shortness of breath and/or chest pain. Your assessment and management should be documented clearly in the notes, however, this should not delay initial clinical assessment, investigations and interventions.Īcute scenarios typically begin with a brief handover from a member of the nursing staff including the patient’s name, age, background and the reason the review has been requested.Any medications or fluids will need to be prescribed at the time (in some cases you may be able to delegate this to another member of staff).Make use of your local guidelines and algorithms in managing specific scenarios (e.g.Review results as they become available (e.g.If you require senior input, call for help early using an appropriate SBARR handoverstructure.Clearly communicate how often would you like the patient’s observations relayed to you by other staff members.All critically unwell patients should have continuous monitoring equipment attached for accurate observations.Make use of the team around you by delegating tasks where appropriate.Re-assess regularly and after every intervention to monitor a patient’s response to treatment.Treat all problems as you discover them.General tips for applying an ABCDE approach in an emergency setting include: You might also be interested in our premium collection of 1,000+ ready-made OSCE Stations, including a range of ABCDE assessment and emergency stations □ Tips before you begin Tracheal deviation away from the affected side: this is a clinical sign of tension pneumothorax and warrants prompt treatment with decompression.Reduced breath sounds on the affected side.Typical clinical signs of a pneumothorax include: A feeling of not being able to take a full breath.Typical symptoms of a pneumothorax include: Tension pneumothoraxĪll types of pneumothorax can potentially develop into a tension pneumothorax.Ī tension pneumothorax is a medical emergency due to the resulting sudden rise in intrathoracic pressure which reduces venous return to the heart and ultimately causes cardiac arrest if left untreated. occurring secondary to penetrating chest trauma).

Pneumothoraces can also be described as spontaneous or traumatic (e.g.

A secondary pneumothorax develops as a result of underlying lung disease such as asthma or COPD.A primary pneumothorax develops in the absence of an underlying disease process.Pneumothoracies can be classified as either primary or secondary:
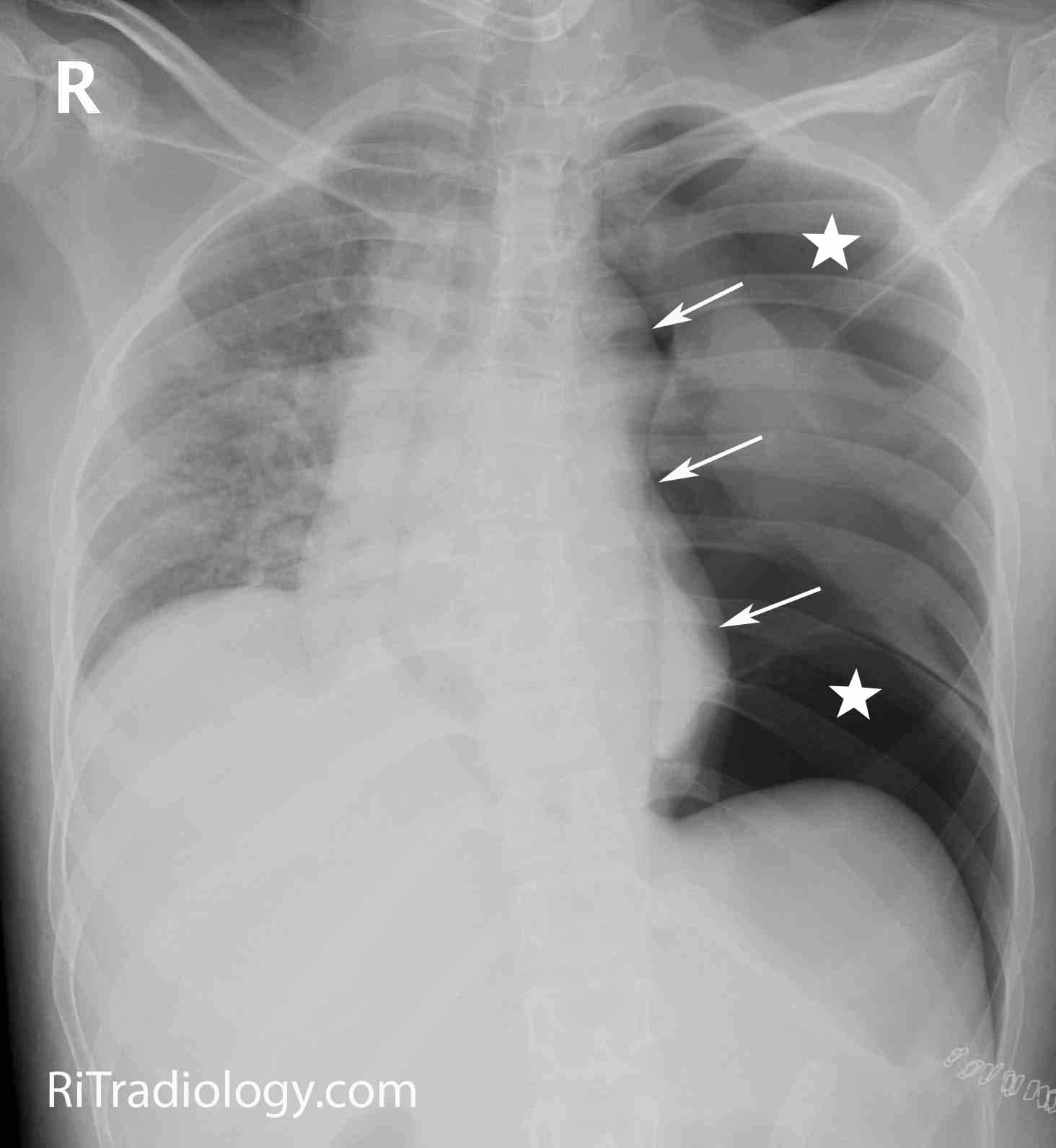
There are several different ways to classify and name pneumothoraces. Clinical features of a pneumothoraxĪ pneumothorax is a collection of air between the parietal and visceral pleura of the lung. You may also be interested in our overview of the ABCDE approach and other emergency management guides.
